New Series: The Science Behind Urban Legends: Fact, Fiction, or Somewhere In-Between?
Think of all the common tales you endured growing up: “An apple a day keeps the doctor away,” “Counting sheep helps you fall asleep” or–a favorite of parents everywhere–“Don’t go outside with wet hair, you’ll catch cold!” Is there truth to these oft-spouted phrases, or are they merely a clever way for parents to coax good behavior from their children?
In our new series, The Science Behind Urban Legends, we’ll search for scientific evidence that supports or refutes these common phrases so that you can decide for yourself.
Starve a Fever, Feed a Cold
Have you ever been so sick that you had absolutely no appetite?
I have, thanks to some bacteria called Streptococcus pyogenes. If you’re familiar with this bug, you’ll probably guess that I had a bad case of strep throat. I spent a week on my couch—body aching, throat red and swollen, and with an extreme aversion to food. When I wasn’t watching reruns of What Not to Wear or wallowing in my own misery, I couldn’t help but ponder this extreme disinterest in eating. Not only was this aversion to food extremely unlike me, but it also seemed counterintuitive to the healing process. Shouldn’t we want to fuel our bodies more when we’re sick to help fight off the infection? Or could not eating actually help us get better?

Should you eat when you’re sick?
As it turns out, it may be true that part of the answer can be gleaned from an old urban legend: “starve a fever, feed a cold.” For scientists’ favorite furry friend, this adage has at least a kernel of truth to it.
A team of researchers led by Ruslan M Medzhitov from the Yale Department of Immunology found that during severe bacterial infections (the “fever” part of the urban legend), not eating helped mice heal faster. However, when the group gave mice a viral flu (analagous to a severe “cold”), starving gave mice only a 10% chance of surviving the infection! But what is so different about these two illnesses that simply changing how mice ate was the difference between life and death? According to Harding Luan, a graduate student in the Medzhitov lab and a co-first author on the paper, it all depends on how these bugs hurt the brain, and how diet helps combat the brain damage.
“There’s a set of stereotypic behaviors that happen when you get infected, like altered sleep patterning, loss of appetite, loss of libido, or lack of grooming,” said Luan. “Everyone knows these, anecdotally—when you’re sick, all these things are true.”
But one response to infection, loss of appetite, was particularly interesting to them.
“The [loss of appetite] is also true in your dog, or flies—even worms stop eating when they’re sick,” said Luan. “We figured this is something so conserved, it must be important.”
The researchers infected mice with the bacterium Listeria monocytogenes, which causes a deadly blood infection called sepsis. Using the septic mouse model, Luan and his co-authors found that feeding during bacterial infection made the mice more likely to die from the infection. More specifically, eating a small amount of sugar made the mice unable to tolerate the symptoms of infection. Although the mice ate only enough sugar to amount to 2% of their daily caloric intake, it was enough to cause them significant damage. The sugar allowed bacteria to produce inflammation, which made cells in the brain die. This cell death led to seizures and eventually killed the mice.
How could something as simple as eating a tiny amount of sugar cause brain malfunction and death during infection? The answer lies in the mouse’s metabolism.
“We can just give a little bit of glucose, and it totally changes [a mouse’s] metabolism. 2% glucose is such a tiny tickle, but when you give that tickle of glucose, it induces a spike of insulin,” said Luan.

Luan explained that this spike of insulin tells the body that there is sugar to eat, which blocks mice from using their fat as fuel. When mice can’t break down their fat, they don’t produce byproducts called ketones. These ketones help mouse brain cells to manage inflammation during infection.
Ketones neutralize inflammatory molecules called reactive oxygen species, molecules that the immune system produces to kill bacteria cells during infection. But if the body makes too many reactive oxygen molecules, it’s the ketones’ job to get rid of them before the molecules hurt host cells.
Feeding the mice sugar during infections blocked this ketone production. The mice didn’t have any ketones, leaving their brain cells defenseless to the inflammatory damage produced by reactive oxygen species.
When they discovered this interesting result in bacterial infections, Luan and his co-authors decided to try another infectious model: viral infection. Since eating was deadly for mice with bacterial infections, Luan expected the same to hold true for mice with viral infections. Surprisingly, the opposite was true. Mice with viral infections were much more likely to survive when force-fed sugar than the infected mice with no food.

“Our premise was that the mice don’t eat during infection, and that helps them survive. So when we saw the opposite with the viral infection, we were so disappointed,” said Luan. “But then we started thinking that maybe it’s important that it’s not true in every case. We started thinking about, for example, if you get sick with a cold, you still want chicken noodle soup. But if you get strep throat for example, and you have a fever, you just want to lay in bed all day and not really eat anything.”
After this result, Luan and his co-authors investigated why the mice with viral and bacterial infections reacted so differently to food.
Luan and his co-authors monitored multiple vital signs and found that the infected mice had decreased body temperatures and breathing rates. This made the researchers suspect some brain damage in the starved mice. Although sugar starvation reduced brain damage during bacterial infections, the same starvation increased brain damage during viral infections.
When a virus infects a cell, it uses the cell as a factory to produce the proteins necessary to copy itself, or produce more virus. If the increase in protein production is too great, the cell can’t keep up with the production and becomes stressed.
“This response seems to have a threshold—the stress can be useful, and help to fix problems in the cell, but when it gets to be too much, then the cell kind of poops out and dies,” said Luan.
To prevent pooping out, mice need sugar during viral infections to deal with the stress of viruses hijacking the protein machinery in their brains.
But to reiterate, sugar is not good during bacterial infections. Even the most miniscule amount of glucose prevents fat breakdown, leaving the brain with no ketones to defend against reactive oxygen species.
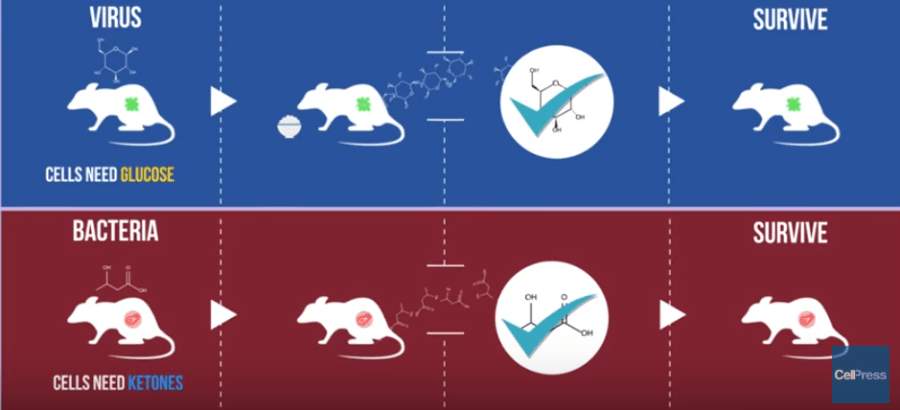
In other words, our urban legend seems to have some truth to it, but maybe we should update it to “Starve a severe, bacterially-induced fever, feed a virally-induced cold.”
Not so fast—despite the convincing findings in mice, Luan recommends that our human readers not change a thing. The Medzhitov lab was alarmed that much of the press coverage on this study suggested that readers change their eating habits when sick. “We were thinking ‘Absolutely not!’ We’re not trying to recommend nutritional advice to anybody!”
So the Medzhitov lab recommends we update the adage to: “Starve a severe, bacterially-induced fever, feed a virally-induced cold—but only if you’re a mouse!” Admittedly, I don’t see this version catching on.
But don’t fret, readers—there may be suggestions for us to follow in the future. Luan informed me that his co-author, Dr. Andrew Wang, is currently leading a clinical trial, changing how he feeds sepsis patients based on this work.
While we still need a lot more research—especially on humans!—I’m still holding out hope that Grandma’s chicken soup may be one of the best cold cures after all.
By Gretchen Wettstein
